In this article, the reader will get a clear idea of the importance of the Liver in our body, its functions, preventive measures for healthy liver and diagnostic methods.
Table of contents
- Introduction
- About the liver
- Liver functions: Understanding the significance of the liver
- How Widespread Is Liver Disease? Look At The Statistics.
- Which risk factors are most commonly associated with liver disease?
- To Look Out For: Symptoms Of Liver Damage?
- Understanding Liver Disease: The Different Stages and What You Need To Know
- Simple Steps for Optimal Liver Health
- Overview of diagnostic methods
- Understanding ALT and AST: How Liver Damage Is Detected Through Blood
- Should You Buy A Self-Test Kit? Here Are Some Pros And Cons To Consider.
- Take-Home Points
- References
Introduction
The Liver is a vital organ with many essential functions, including breaking down toxins, aiding digestion, and storing essential nutrients.
Liver disease is a significant health problem worldwide that can be caused by excessive alcohol consumption, obesity, and Chronic liver inflammation.
Symptoms of liver disease can include jaundice, fatigue, nausea and vomiting, abdominal pain, loss of appetite, weight loss, dark urine, or pale stool.
It is vital to eat a healthy diet, exercise regularly, maintain a healthy weight, limit alcohol consumption, and avoid exposure to toxins.
Diagnostic methods most commonly used to examine liver diseases are blood tests, imaging tests, liver biopsy, endoscopic procedures and self-blood tests.

About the liver
The Liver is situated in the upper right part of the abdomen, just below the diaphragm. It presents about 2% of the body mass1 and weighs about 1,5 kg2.
The Liver is composed of several cell types organised around lobules – hexagonally shaped functional units that form the liver tissue.3 Each of these cell types has a distinct function and they work together to enable liver functioning.
The largest parts of the liver are the right and the left lobes. Additionally to these two parts, the liver also has caudate and quadrate lobes.4
Liver gets about 75-80% of blood via portal vein and about 20-25% via the hepatic artery.4 The hepatic artery brings oxygenated blood while the portal vein brings blood rich in nutrients and antigens from the gastrointestinal system.5
Hepatic veins collect the blood from the liver and take them to the inferior vena cava which transports it back to the heart.5
Gallbladder is a pear-shaped organ under the liver. It is a part of the biliary system and stores bile which the liver produces.6
References:
- Kalra A, Yetiskul E, Wehrle CJ, et al. Physiology, Liver. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-.
- Molina DK, DiMaio VJ. Normal organ weights in men: part II-the brain, lungs, liver, spleen, and kidneys. Am J Forensic Med Pathol. 2012 Dec;33(4):368-72.
- Trefts E, Gannon M, Wasserman DH. The liver. Curr Biol. 2017 Nov 6;27(21):R1147-R1151.
- Vernon H, Wehrle CJ, Alia VSK, et al. Anatomy, Abdomen and Pelvis, Liver. [Updated 2022 Nov 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-.
- Lorente S, Hautefeuille M, Sanchez-Cedillo A. The liver, a functionalized vascular structure. Sci Rep. 2020 Oct 1;10(1):16194.
- Jones MW, Small K, Kashyap S, et al. Physiology, Gallbladder. [Updated 2022 May 8]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2022 Jan-.
Liver functions: Understanding the significance of the liver
To understand the significance of the liver in our body, we need to summarise the liver’s primary functions.
Liver has over 500 functions1 that keep us healthy and enable our body normal functioning.
One of its prominent roles is metabolism, which involves breaking down nutrients from food into usable energy for the body.
The liver also acts as a blood reservoir, storing extra blood that can be released when needed by the body.
Another vital function of the liver is bile production and secretion, which helps digest fats and remove waste products from the body.2
Additionally, it plays a critical role in immune function by removing harmful toxins from the bloodstream.
In addition to these crucial functions, the liver also stores vitamins such as A, D, E, and K and produces proteins necessary for blood clotting.
It’s clear that without this organ’s many contributions to our health, we would not be able to survive.
Metabolism
The liver plays a crucial role in nutrient metabolism, the process of breaking down food and turning it into energy that our bodies can use. In addition to fat metabolism, the liver also helps to metabolize proteins and amino acids.3
The liver helps to regulate blood sugar levels by storing glucose as glycogen when levels are high and releasing it back into the bloodstream when levels drop.4
The liver is also responsible for processing drugs and toxins, converting them into forms that can be safely eliminated from the body.2 This detoxification process is essential for maintaining overall health and preventing disease.
Blood Reservoir
The liver can hold about 12% of the body’s total blood volume. Half of the blood volume reserves can be excreted at any given time.5
When there is a sudden decrease in blood pressure or significant loss of blood due to injury, the liver releases stored blood into circulation to help maintain stable levels and prevent shock. This process ensures that vital organs like the brain and heart receive enough oxygenated blood to function properly.6
Furthermore, there is increased demand for oxygenated blood in muscles during exercise or physical activity. The liver helps meet this demand by releasing stored blood into circulation when needed.
Bile Production
The liver produces bile, which is a greenish-yellow fluid that helps in digestion by breaking down fats into smaller molecules through the process called emulsification.7
During the meal, the bile produced by the liver flows directly into the small intestine, where it is mixed with food.8
The total bile flow in a day is approximately 600 ml. When it is not needed, the bile travels through small tubes called bile ducts to reach the gallbladder, where it is stored until needed for digestion.7
When food containing fat enters the small intestine, hormones signal the gallbladder to release bile into the digestive tract.7
Bile not only helps in digesting fats but also aids in the removal of waste products from our bodies.2
It contains bilirubin, which is formed when red blood cells break down. Bilirubin gives feces its characteristic brown color.7
If there is any interruption in the flow of bile due to an obstruction or blockage in one of the ducts leading from your liver or gallbladder, it can result in health problems like jaundice or cholecystitis.9
Immune Function
The liver plays a crucial role in the body’s immune function. It contains specialized cells that help to identify and destroy foreign substances, including bacteria, viruses, and toxins.10
The imperative role in maintaining liver functions have Kupfer cells, which are the first innate immune cells and protect the liver from bacterial infections.11
These cells work together with other immune cells throughout the body to provide overall protection against disease.
One of the primary functions of the liver is to filter blood. During this process, any harmful microbes or toxins present in the bloodstream are identified and neutralized by immune cells within the liver.12
However, if there is an overwhelming amount of foreign material entering our bodies, like heavy alcohol consumption or viral infection, it may lead to a compromised function of these specialized immune cells, thus leading us to be poorly protected against diseases.
Vitamin Storage
The liver plays a crucial role in the storage of essential vitamins that are vital for our overall health and well-being.
It stores various types of vitamins, including Vitamin A, D, E, K and B12. These vitamins are essential for maintaining healthy skin, bones, eyesight and blood cells.13
Vitamin A is stored in the form of retinol in the liver. It helps to maintain good vision, healthy skin and mucous membranes. Vitamin A deficiency can cause vision, skin, bone and immunity disorders. Excess of vitamin A can lead to excess collagen production, fibrosis and liver injury.13
The liver also stores Vitamin D, which is essential for strong bones as it helps to absorb calcium from food.14
Vitamin E is a potent antioxidant that protects the body cells against oxidative stress, and it helps regulate immune function and balances normal coagulation.14
The liver also plays a significant role in storing Vitamin K, which aids blood clotting by promoting the production of clotting factors and anticoagulant proteins.14
Humans cannot synthesize vitamin B12, but it can be obtained from animal sources such as dairy products and meat. The liver stores this vitamin along with other B-complex vitamins that help convert food and support normal growth.14
References:
- Bhatia SN, Underhill GH, Zaret KS, Fox IJ. Cell and tissue engineering for liver disease. Sci Transl Med. 2014 Jul 16;6(245):245sr2.
- Kalra A, Yetiskul E, Wehrle CJ, et al. Physiology, Liver. [Updated 2023 May 1]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Trefts E, Gannon M, Wasserman DH. The liver. Curr Biol. 2017 Nov 6;27(21):R1147-R1151.
- Nakrani MN, Wineland RH, Anjum F. Physiology, Glucose Metabolism. [Updated 2022 Jul 25]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Greenway CV, Lautt WW. Hepatic circulation. In: Schultz SG, Wood JD, Rauner BB, editors. Handbook of Physiology. The Gastrointestinal System I. Part 2, Chapter 41. Vol. 1. American Physiological Society; New York: Oxford University Press; 1989. pp. 1519–64.
- Lautt WW. Hepatic Circulation: Physiology and Pathophysiology. San Rafael (CA): Morgan & Claypool Life Sciences; 2009. Chapter 2, Overview.
- Hundt M, Basit H, John S. Physiology, Bile Secretion. [Updated 2022 Sep 26]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- InformedHealth.org [Internet]. Cologne, Germany: Institute for Quality and Efficiency in Health Care (IQWiG); 2006-. How does the gallbladder work? 2010 Jan 21 [Updated 2018 Sep 6].
- Joseph A, Samant H. Jaundice. [Updated 2023 Feb 12]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Kubes P, Jenne C. Immune Responses in the Liver. Annu Rev Immunol. 2018 Apr 26;36:247-277.
- Nguyen-Lefebvre AT, Horuzsko A. Kupffer Cell Metabolism and Function. J Enzymol Metab. 2015;1(1):101.
- Maher JJ. Exploring alcohol’s effects on liver function. Alcohol Health Res World. 1997;21(1):5-12.
- LiverTox: Clinical and Research Information on Drug-Induced Liver Injury [Internet]. Bethesda (MD): National Institute of Diabetes and Digestive and Kidney Diseases; 2012-. Vitamins.
- Khazai N, Judd SE, Tangpricha V. Calcium and vitamin D: skeletal and extraskeletal health. Curr Rheumatol Rep. 2008 Apr;10(2):110-7.

How Widespread Is Liver Disease? Look At The Statistics.
Liver disease is a significant public health problem in Europe and worldwide.5 It is the fifth most common cause of death in the European Union (EU) and the third most common cause of death in the WHO European Region.
Approximately 2 million deaths occur annually from liver diseases, with cirrhosis and viral hepatitis/hepatocellular carcinoma each contributing 1 million fatalities.
Cirrhosis is the 11th most common cause of death worldwide, and liver cancer is the 16th leading cause; they account for 3.5% of global mortality.6
Alcohol consumption is a significant risk factor on a global scale, with over 75 million people suffering from alcohol-use disorders and at risk of its resulting liver disease.
Obesity/overweight (2 billion adults) and diabetes (400 million) are further linked to non-alcoholic fatty liver disease and hepatocellular carcinoma.7 There remains a high prevalence of viral hepatitis.
Chronic infection with the Hepatitis B virus and Hepatitis C virus is a primary cause of chronic liver disease, cirrhosis, and hepatocellular carcinoma.
According to ECDC data in 2017, 4.7 million people were living with chronic hepatitis B virus infection and 3.9 million people with Hepatitis C infection in EU/EEA countries and the UK.
In the EU/EEA, deaths attributed to the hepatitis B virus and hepatitis C virus are estimated to account for around 55% of liver cancer deaths and 45% of all deaths due to cirrhosis and other chronic liver diseases.
At the same time, drug-induced hepatic injury continues to rise as a significant source of acute hepatitis.8

Which risk factors are most commonly associated with liver disease?
Multiple risk factors can lead to the development of liver disease. Understanding them is crucial for preventive measures and maintaining liver health.
- Excessive alcohol consumption: A well-known risk factor for liver damage.
- Genetic factors: Specific genetic mutations can increase the likelihood of developing fatty liver disease, cirrhosis, and liver cancer.
- Lifestyle Factors: Unhealthy diet, lack of exercise, smoking, drug abuse, unsafe sexual practices, stress.
- Viral infections: Hepatitis B and C are major causes of chronic liver disease.
- Environmental factors: Exposure to toxins and chemicals can also impact liver function.
- Obesity and Metabolic syndrome: Increases the risk of hepatic inflammation and fibrosis progression, leading to NASH-related cirrhosis.
- Other medical conditions: Hemochromatosis (an excess of iron in the body) and Wilson’s disease (a disorder that prevents the body from adequately metabolising copper) can lead to Liver damage.

By understanding these risk factors, individuals can make informed choices about their lifestyle habits, seek appropriate medical care when necessary, and take steps towards preventing or managing potential complications related to their liver health.
Alcohol Consumption
Alcohol consumption is one of the most significant risk factors for liver disease. Excessive and chronic alcohol use can lead to liver problems, including fatty liver disease, alcoholic hepatitis, and cirrhosis.1
When you consume alcohol, your liver works hard to break it down and eliminate it from your body. However, excessive drinking over time can overwhelm the liver’s ability to process alcohol efficiently. This can result in inflammation and damage to liver cells.2
Heavy drinkers are at a higher risk of developing fatty liver disease, which involves an abnormal buildup of fat in the liver cells. If left untreated, this condition can progress to more severe forms of liver damage.1
Another consequence of excessive alcohol consumption is alcoholic hepatitis, which is characterised by inflammation and swelling of the liver. This condition can cause symptoms such as jaundice, malaise, tender hepatomegaly, and subtle features of systemic inflammatory response.3
The most severe form of alcohol-related liver disease is cirrhosis. This occurs when healthy tissue in the liver is replaced by scar tissue due to long-term alcohol abuse. Cirrhosis impairs the normal functioning of the organ and may eventually lead to complete failure.4
It’s important to note that not everyone who drinks heavily will develop significant liver damage. However, certain factors increase an individual’s susceptibility to alcohol-related harm to their liver. These include genetic predisposition, family history of alcoholic-related diseases, and co-existing medical conditions like viral hepatitis or obesity.
To protect your health and reduce your risk of developing severe complications related to alcohol consumption:
- Limit your alcohol intake: Follow recommended guidelines for moderate drinking – no more than one drink per day for women and two for men.5
- Seek support: If you’re struggling with controlling your drinking habits or have developed alcohol addiction, contact a healthcare professional or support group.
- Stay informed: Learn about the potential consequences of alcohol abuse, read literature and follow guidelines to overcome the threat.
Genetic Factors
Genetic factors play a significant role in increasing the risk of developing liver disease.
Our genes determine how our bodies function, including how our liver performs its functions.
Certain genetic variations can make individuals more susceptible to liver damage or impair their ability to repair damaged liver cells.6
One example of a genetic factor that increases the risk of liver disease is a condition called hereditary hemochromatosis.6 This disorder causes excessive iron absorption by the body, leading to iron overload in various organs, including the liver.7
Another genetic factor associated with an increased risk of liver disease is alpha-1 antitrypsin deficiency (AATD). AATD is an inherited disorder that affects the lungs and liver. In some cases, abnormal proteins produced due to AATD accumulate in the liver cells, damaging the liver.8
There are also other genetic predispositions such as Wilson’s disease, Gilbert syndrome, Crigler‐Najjar syndrome.6
It’s vital for individuals with a family history of these genetic conditions or other known genetic predispositions for liver disease to be aware of their increased risk.
Regular check-ups and screenings can help detect any early signs of liver damage and allow for prompt intervention.
Lifestyle Factors
Certain habits and behaviours can cause long-term damage to the liver by putting unnecessary strain on it. Here are some lifestyle factors that you should be aware of:9,10,11,12
- Unhealthy Diet: Consuming a diet high in processed foods, saturated fats, and added sugars can contribute to developing fatty liver disease. A balanced diet of fruits, vegetables, whole grains, and lean proteins is essential for maintaining a healthy liver.
- Lack of Exercise: Leading a sedentary lifestyle promotes weight gain and increases the risk of developing non-alcoholic fatty liver disease (NAFLD). Regular physical activity helps burn excess fat and reduces the accumulation of harmful substances in the liver.
- Smoking: Smoking is known to have detrimental effects on various organs in the body, including the liver. It correlates to an increased risk of alcoholic cirrhosis and hepatocellular carcinoma (the most common form of primary liver cancer).
- Drug Abuse: The misuse or abuse of drugs such as alcohol or illicit substances puts immense stress on the liver and can lead to irreversible damage over time.
- Unsafe Sexual Practices: Engaging in unprotected sex or having multiple sexual partners increases your chances of contracting sexually transmitted infections like hepatitis B and C – both significant contributors to chronic hepatitis and subsequent complications.
- Stress Management:13 Chronic stress has been associated with several health issues, including inflammation, which may negatively impact overall organ function, including that of our vital organ–the liver!
By adopting healthier lifestyle choices such as eating nutritious foods, staying physically active, and avoiding smoking/drug abuse/unprotected sex practices while managing stress effectively – we significantly reduce our risks! Taking small daily steps towards positive changes will go a long way in safeguarding our liver.
Viral Infections
Viral infections play a significant role in the development of liver disease. Several viruses are known to directly target and attack the liver, causing inflammation and damage.
Hepatitis viruses, including Hepatitis A, B, C, D, E, G are some of the most common viral infections that can lead to liver disease:14
- Hepatitis A is typically spread through contaminated food or water. While it usually resolves on its own without causing long-term damage to the liver, severe cases may result in acute liver failure.
- Hepatitis B and C are transmitted through contact with infected blood or bodily fluids. These viruses can cause chronic hepatitis if left untreated and may progress to more severe conditions such as cirrhosis or liver cancer.
- Hepatitis D only occurs in individuals already infected with hepatitis B and can worsen the effects of both viruses on the liver.
- Hepatitis E is primarily transmitted through contaminated water sources in areas with poor sanitation. It often causes self-limiting acute hepatitis but can be severe in pregnant women.
- Hepatitis G is common and present all around the world. People are mostly asymptomatic or can have mild infection.
Furthermore, several other viral infections can indirectly impact liver health such as Viral hemorrhagic fevers (VHFs), varicella-zoster virus (VZV), Human Herpesviruses, Epstein-Barr virus (EBV) and cytomegalovirus (CMV).15
Environmental Factors
Exposure to toxins and chemicals present in our surroundings can have detrimental effects on the liver.
Toxic substances can be found in polluted air, industrial waste, household cleaning products, and even in certain medications. Prolonged exposure to these toxins can lead to liver damage.16
Consuming food or water that is contaminated with viruses like Hepatitis A or E can result in viral hepatitis, which is a common cause of liver disease.14
Occupational hazards such as working with hazardous materials or being exposed to certain chemicals regularly can also increase the likelihood of developing liver problems.
Living in areas with high levels of heavy metals like arsenic or cadmium in drinking water or soil contamination from industrial activities has been associated with an increased risk of liver disease.17
It’s important to be aware of these environmental factors and take necessary precautions to minimise their impact on your health.
Regularly check for updates on air quality alerts and avoid exposure to harmful substances whenever possible.
Drinking clean and filtered water and consuming fresh and organic foods can help reduce the risk posed by contaminants.
Obesity and Metabolic Syndrome
Obesity and metabolic syndrome are risk factors that significantly contribute to liver disease development.
Obesity, characterised by excess body fat, stresses the liver. An excessive accumulation of fat in the liver cells can lead to a condition called non-alcoholic fatty liver disease (NAFLD). If left untreated, NAFLD is becoming increasingly prevalent and can progress to more severe conditions such as cirrhosis or even liver cancer.18
Metabolic syndrome (MetS) refers to a cluster of conditions, including high blood pressure, obesity, insulin resistance, and atherogenic dyslipidemia.19
The exact mechanisms linking obesity and metabolic syndrome to liver disease are still being researched. However, it is believed that insulin resistance plays a key role.20
Insulin resistance (also known as impaired insulin sensitivity) occurs when our bodies become less responsive to the insulin hormone. Insulin resistance is primarily an acquired condition related to excess body fat,21 and the condition leads to increased storage of fat in the liver22.
Healthy lifestyle practices such as regular exercise and a balanced diet can help manage weight issues and reduce the risk of metabolic syndrome-associated complications like fatty liver disease.
Maintaining normal blood pressure levels and managing diabetes effectively also play important roles in preserving optimal liver health.
It’s crucial for individuals with higher weight or have symptoms related to metabolic syndrome to consult their healthcare provider for proper diagnosis, guidance on lifestyle changes, and necessary medical interventions if required.
By addressing these underlying causes, we can minimise the risk factors for developing severe forms of liver diseases associated with obesity and metabolic syndrome.
Other Medical Conditions
Several medical conditions may directly affect the liver or indirectly contribute to its dysfunction.
One such condition is autoimmune hepatitis, which occurs when the body’s immune system mistakenly attacks the liver cells. The exact cause is unknown. This can lead to inflammation and damage, increasing the risk of liver disease.23
Chronic viral infections such as hepatitis B and C can also cause long-term damage to the liver if left untreated. These infections are often asymptomatic for many years, making regular screenings crucial in identifying them early on.14
Certain metabolic disorders, such as hemochromatosis (excessive iron buildup) or Wilson’s disease (abnormal copper accumulation), can result in liver damage over time.6
Additionally, non-alcoholic steatohepatitis (NASH), a severe form of fatty liver disease, can progress to cirrhosis if not addressed promptly.4
Liver diseases are also commonly associated with other health conditions like diabetes and high blood pressure. These comorbidities further increase the risk and severity of liver-related complications.24
Individuals with any underlying medical condition need to work closely with their doctor in managing their overall health while keeping a close eye on their liver function through regular check-ups and screenings.
By addressing these medical conditions proactively, it becomes possible to minimise the risks associated with liver diseases.
References:
- Osna NA, Donohue TM Jr, Kharbanda KK. Alcoholic Liver Disease: Pathogenesis and Current Management. Alcohol Res. 2017;38(2):147-161.
- Donohue TM Jr. Alcohol-induced steatosis in liver cells. World J Gastroenterol. 2007 Oct 7;13(37):4974-8.
- Shah NJ, Royer A, John S. Alcoholic Hepatitis. [Updated 2023 Jan 2]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Sharma B, John S. Hepatic Cirrhosis. [Updated 2022 Oct 31]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Rehm J. The risks associated with alcohol use and alcoholism. Alcohol Res Health. 2011;34(2):135-43.
- Weber SN, Lammert F. Genetics in liver diseases: From diagnostics to precise therapy. Clin Liver Dis (Hoboken). 2017 Feb 3;9(1):1-4.
- Kowdley KV. Iron Overload in Patients With Chronic Liver Disease. Gastroenterol Hepatol (N Y). 2016 Nov;12(11):695-698.
- Meseeha M, Attia M. Alpha-1 Antitrypsin Deficiency. [Updated 2023 Feb 7]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Nivukoski U, Niemelä M, Bloigu A, Bloigu R, Aalto M, Laatikainen T, Niemelä O. Combined effects of lifestyle risk factors on fatty liver index. BMC Gastroenterol. 2020 Apr 15;20(1):109.
- Sahlman P, Nissinen M, Puukka P, Jula A, Salomaa V, Männistö S, Lundqvist A, Valsta L, Perola M, Färkkilä M, Åberg F. Genetic and lifestyle risk factors for advanced liver disease among men and women. J Gastroenterol Hepatol. 2020 Feb;35(2):291-298.
- Pang Y, Han Y, Yu C, Kartsonaki C, Guo Y, Chen Y, Yang L, Du H, Hou W, Schmidt D, Stevens R, Chen J, Chen Z, Lv J, Li L. The role of lifestyle factors on comorbidity of chronic liver disease and cardiometabolic disease in Chinese population: A prospective cohort study. Lancet Reg Health West Pac. 2022 Aug 10;28:100564.
- Nivukoski U, Niemelä M, Bloigu A, Bloigu R, Aalto M, Laatikainen T, Niemelä O. Impacts of unfavourable lifestyle factors on biomarkers of liver function, inflammation and lipid status. PLoS One. 2019 Jun 20;14(6):e0218463.
- Vere CC, Streba CT, Streba LM, Ionescu AG, Sima F. Psychosocial stress and liver disease status. World J Gastroenterol. 2009 Jun 28;15(24):2980-6. doi: 10.3748/wjg.15.2980.
- Mehta P, Reddivari AKR. Hepatitis. [Updated 2022 Oct 24]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Spengler U, Fischer HP, Caselmann WH. Liver Disease Associated with Viral Infections. Zakim and Boyer’s Hepatology. 2012:629–43.
- Barouki R, Samson M, Blanc EB, Colombo M, Zucman-Rossi J, Lazaridis KN, Miller GW, Coumoul X. The exposome and liver disease – how environmental factors affect liver health. J Hepatol. 2023 Mar 6:S0168-8278(23)00166-6.
- Hong D, Min JY, Min KB. Association Between Cadmium Exposure and Liver Function in Adults in the United States: A Cross-sectional Study. J Prev Med Public Health. 2021 Nov;54(6):471-480.
- Liu Q, Bengmark S, Qu S. The role of hepatic fat accumulation in pathogenesis of non-alcoholic fatty liver disease (NAFLD). Lipids Health Dis. 2010 Apr 28;9:42.
- Rochlani Y, Pothineni NV, Kovelamudi S, Mehta JL. Metabolic syndrome: pathophysiology, management, and modulation by natural compounds. Ther Adv Cardiovasc Dis. 2017 Aug;11(8):215-225.
- Saltiel AR, Olefsky JM. Inflammatory mechanisms linking obesity and metabolic disease. J Clin Invest. 2017 Jan 3;127(1):1-4.
- Freeman AM, Pennings N. Insulin Resistance. [Updated 2022 Sep 20]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Trouwborst I, Bowser SM, Goossens GH, Blaak EE. Ectopic Fat Accumulation in Distinct Insulin Resistant Phenotypes; Targets for Personalized Nutritional Interventions. Front Nutr. 2018 Sep 4;5:77.
- Linzay CD, Sharma B, Pandit S. Autoimmune Hepatitis. [Updated 2022 Aug 22]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan-.
- Garcia-Compean D, Jaquez-Quintana JO, Gonzalez-Gonzalez JA, Maldonado-Garza H. Liver cirrhosis and diabetes: risk factors, pathophysiology, clinical implications and management. World J Gastroenterol. 2009 Jan 21;15(3):280-8.
To Look Out For: Symptoms Of Liver Damage?
The symptoms of liver damage vary from mild to severe, and they can often go unnoticed until it is too late.
The most common symptoms of Liver damage are fatigue, nausea, vomiting, abdominal pain, loss of appetite, weight loss, dark urine, and pale stool.11
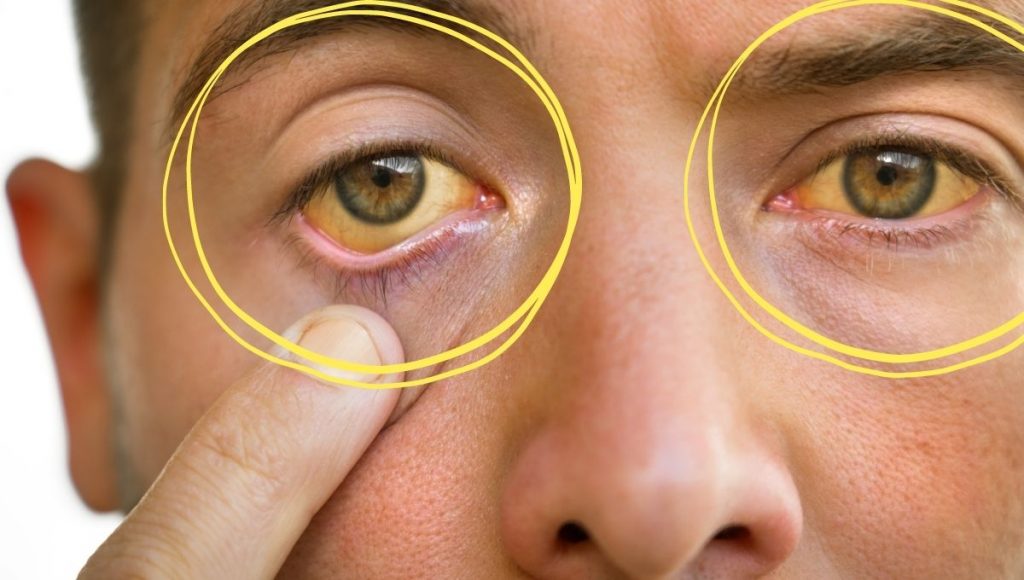
Jaundice: this happens due to increased bilirubin in the blood, which causes skin and eyes to turn yellow.
Fatigue: A state of exhaustion characterised by extreme tiredness and energy depletion.
Nausea and Vomiting: An increase in toxins in the blood or digestive issues caused by liver inflammation can cause nausea and vomiting.
Abdominal Pain: Inflammation or enlargement of the Liver causes abdominal pain.
Loss of appetite: Loss of appetite or inability to absorb nutrients properly can cause weight loss.
Dark urine: Blood bilirubin may cause dark urine.
Pale stool: The lack of bile in the stool can be caused by liver damage.
Understanding Liver Disease: The Different Stages and What You Need To Know
There are four stages of liver disease Hepatitis (inflammation), Fibrosis(scarring), Cirrhosis(Severe scarring), and Liver failure.
Early diagnosis of liver disease will help you assess any liver-related issues.
It is important to recognise the stages of liver disease and to be aware of the signs and symptoms at each stage. Knowing the stages of liver disease can help you identify potential issues early and take action to prevent further damage.
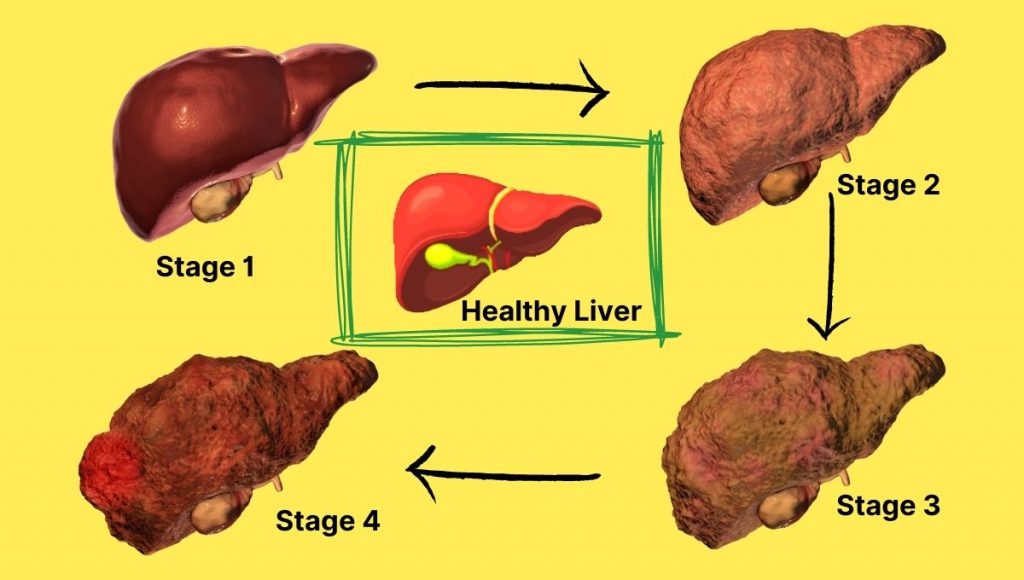
Stage 1: Inflammation
The Liver handles the toxic waste that enters our bodies. When the Liver cannot handle or remove toxins from the body, the body reacts with inflammation, swelling the organ. As inflammation is a sign of viral hepatitis or immune hepatitis, alcoholic fatty Liver or non-alcoholic fatty Liver, it is crucial to see a doctor as soon as possible.
Stage 2: Scarring
When the Liver is left untreated, inflammation can cause scarring to the Liver. Scarred tissue does not function as well as healthy tissue, making the organ less efficient. This is referred to as Fibrosis.
Stage 3: Cirrhosis
The 3rd stage of liver disease, Liver Cirrhosis, is characterised by severe scarring and an inability to heal. This process can take decades, providing ample opportunity to act before things become critical.
Stage 4: Liver Failure or End-stage liver disease (ESLD)
This is the final stage. It can take years for the Liver to reach this stage when it stops functioning completely, as it cannot heal itself. There are two types of liver failure. The acute form occurs within 48 hours after the poison is absorbed in the body or after a drug overdose. The chronic condition evolves when alcohol poisons your Liver – the most common cause of liver transplantation.
Simple Steps for Optimal Liver Health
Maintaining a healthy liver is very important as the Liver is one of the most important organs which performs major functions in our body.
Other than taking medicines or getting surgery or transplantation, we can take care of the Liver by following these very simple tasks:
- Maintaining a healthy diet can help you keep your Liver healthy and clean.12
- Doing regular physical activities can help you keep your Liver healthy.
- You can keep your Liver healthy by keeping your weight according to BMI (Body Mass Index) standards.
- Consumption of alcohol is a significant cause of liver diseases, so avoid high alcohol consumption.
- You can take some preventive measures to avoid liver dysfunction, for example, getting a vaccination against Hepatitis A and B etc.

Overview of diagnostic methods
Research has shown that early detection and prompt treatment of liver problems can significantly reduce the risk of liver failure or cancer.
A blood test can help to recognise major liver problems by checking the AST and ALT ratios. Moreover, a self-blood test for the Liver is a simple procedure you can do in the comfort of your home.

Imaging tests like Ct scan, MRI scan, and Ultrasound scan for the Liver are frequently performed to examine the Liver’s physiological status.13

Liver biopsy is also an effective diagnostic method but an invasive method in which a needle is inserted into your Liver. A small quantity of liver cells is taken and sent to a lab to check the development of scarring in the Liver, which happens in the second and third stage of liver disease.14

The endoscopic procedure is done in the final stage of liver disease to check the development of cirrhosis in the Liver.
Understanding ALT and AST: How Liver Damage Is Detected Through Blood
AST and ALT are enzymes found in many tissues in the body but are most abundant in the Liver.
When the Liver is damaged, ALT and AST enzymes leak from the Liver into the bloodstream. This results in a raised concentration of ALT/AST in the blood.
- ALT (alanine aminotransferase) is an enzyme that breaks down fats in the Liver. As a result of these chemical reactions, your Liver produces bile, which breaks down food and toxins and fights infection.15
- AST (aspartate aminotransferase) is an enzyme that plays a vital role in many metabolic processes in our body.16
AST is found in the blood at higher levels when there is damage to the liver cells, while ALT is found in the blood at higher levels when there is inflammation of the Liver.
The concentration of these liver enzymes can be measured with a simple blood test which can give important information about your Liver’s health.17
If you experience symptoms of liver dysfunction or other diseases, your healthcare provider will first check the concentration of liver enzymes.
Increased ALT and AST and their ratios are used in clinical practice to diagnose specific diseases.18
For example, the De Ritis ratio also referred to as the AST/ALT ratio was first proposed for hepatitis diagnosis and is commonly applied for distinguishing between fatty liver conditions.
Furthermore, the AST/ALT ratio is a reliable predictor of non-liver diseases such as cardiovascular disease, certain cancers, and type 2 diabetes mellitus.18

Should You Buy A Self-Test Kit? Here Are Some Pros And Cons To Consider.
A liver self-test is an easy, fast and inexpensive method for assessing liver function.
Pros of the Liver Home Test
- It is easy to use. You can perform the analysis by yourself at home.
- There is no need to send a sample to a laboratory.
- Self-testing is relatively inexpensive. Usually, it is much more cost effective than traditional methods of testing.
- The results are available within minutes.
Cons of the Liver Home Test
- The liver function self-test is not 100% accurate. There is a slight chance that the test will give a false positive or false negative result.
- It is impossible to control if someone collects the sample properly at home. People should always strictly follow the instructions for use.
- Rapid tests are unable to quantify the concentration of liver enzymes. It is only possible with laboratory analysis.
- AST/ALT self-tests for the Liver may only be available in some areas.
- The self-blood test for the Liver is invasive.
- The insurance may not cover the test, so you must bear the cost. At your physician, you might get it for free.
-
 Liver Function Home Test (ALT and AST)14.18 € incl. VAT
Liver Function Home Test (ALT and AST)14.18 € incl. VAT
You should always purchase the test kit from a reputable source. Reliability and testing experience can differ significantly between various brands.
Take-Home Points
- The Liver is a vital organ which deals with some significant functions in our body.
- Maintaining a healthy liver in your body is simple. Follow a well-balanced and healthy diet, avoiding toxin intake, alcohol intake etc.
- The symptoms of liver dysfunction vary from mild to severe, and they can often go unnoticed until it is too late.
- Fatigue, nausea, vomiting, abdominal pain, loss of appetite, weight loss, dark urine, and pale stool are symptoms of liver dysfunction.
- There are four stages of liver disease: Stage 1 – Hepatitis (Inflammation), Stage 2 – Fibrosis (Scarring), Stage 3 – Cirrhosis (Severe scarring), and Stage 4 – Liver failure.
- Aspartate transaminase (AST) and alanine aminotransferase (ALT) are biomarkers that the Health care provider checks first in case of any symptoms or dysfunctions in your body.
- Advancement of medical technology, getting a self-blood test for the Liver is now possible.
- Self-test for the Liver has pros and cons. Consider them before buying any self-tests.

References
- Saxena R, Theise ND, Crawford JM. Microanatomy of the human liver-exploring the hidden interfaces. Hepatology. 1999 Dec;30(6):1339-46. doi: 10.1002/hep.510300607. PMID: 10573509.
- Menche N. (ed.) Biologie Anatomie Physiologie. Munich: Urban & Fischer/ Elsevier; 2012.
- Pschyrembel W. Klinisches Wörterbuch. Berlin: De Gruyter; 2014.
- Schmidt R, Lang F, Heckmann M. Physiologie des Menschen: mit Pathophysiologie. Heidelberg: Springer; 2011.
- Jewell J, Sheron N. Trends in European liver death rates: implications for alcohol policy. Clin Med (Lond). 2010 Jun;10(3):259-63. doi: 10.7861/clinmedicine.10-3-259. PMID: 20726458; PMCID: PMC5873553.
- “The Burden of Liver Disease in Europe: A Review of Available Epidemiological Data.” Journal of Hepatology, vol. 58, no. 3, 2013, pp. 593–608. https://doi.org/10.1016/j.jhep.2012.12.005.
- Mokdad, A. A., et al. “& Naghavi, M.(2014). Liver cirrhosis mortality in 187 countries between 1980 and 2010: a systematic analysis.” BMC medicine 12.1: 145.
- Monitoring of responses to the hepatitis B and C epidemics in EU/EEA countries – 2020 data (2022) European Centre for DiseasePreventionandControl.Availableat:https://www.ecdc.europa.eu/en/news-events/monitoring-responses-hepatitis-b-and-c-epidemics-eueea-countries-2020-data (Accessed: February 10, 2023).
- Pimpin, Laura, et al. “Burden of liver disease in Europe: epidemiology and analysis of risk factors to identify prevention policies.” Journal of hepatology 69.3 (2018): 718-735.
- Majid B, Khan R, Junaid Z, Khurshid O, Rehman SH, Jaffri SN, Zaidi B, Zehra J, Batool S, Altaf S, Jatoi A, Safina F. Assessment of Knowledge About the Risk Factors of Chronic Liver Disease in Patients Admitted in Civil Hospital Karachi. Cureus. 2019 Oct 20;11(10):e5945. doi: 10.7759/cureus.5945. PMID: 31799087; PMCID: PMC6860746.
- Newton, Julia L., and David EJ Jones. “Managing systemic symptoms in chronic liver disease.” Journal of hepatology 56 (2012): S46-S55.https://doi.org/10.1016/S0168-8278(12)60006-3
- Mega A, Marzi L, Kob M, Piccin A, Floreani A. Food and Nutrition in the Pathogenesis of Liver Damage. Nutrients. 2021 Apr 16;13(4):1326. doi: 10.3390/nu13041326. PMID: 33923822; PMCID: PMC8073814.
- Hall P, Cash J. What Is the Real Function of Liver ‘Function’ Tests? (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3609680/) Ulster Med J. 2012; 81(1):30-36.
- Lala V, Goyal A, Bansal P, Minter, DA. Liver Function Tests. (https://www.ncbi.nlm.nih.gov/books/NBK482489/) StatPearls. Updated July 4, 2020.
- Ida M. Washington, Gerald Van Hoosier, in The Laboratory Rabbit, Guinea Pig, Hamster, and Other Rodents, 2012
- Otto-Ślusarczyk D, Graboń W, Mielczarek-Puta M. Aminotransferaza asparaginianowa–kluczowy enzym w metabolizmie ogólnoustrojowym człowieka [Aspartate aminotransferase–key enzyme in the human systemic metabolism]. Postepy Hig Med Dosw (Online). 2016 Mar 16;70:219-30. Polish. doi: 10.5604/17322693.1197373. PMID: 27117097.
- Nidhi Raval, … Rakesh K. Tekade, in Biomaterials and Bionanotechnology, 2019
- Giannini EG, Testa R, Savarino V. Liver Enzyme Alteration: A Guide for Clinicians. (https://www.ncbi.nlm.nih.gov/pmc/articles/PMC545762/) CMAJ. 2005;172(3):367-379.